News and Award
About CMUH
When Seconds Matter: Redesigning Critical Care for the Modern ICU
At 3 a.m., an ICU tells the truth. You hear the rhythm of monitors and the quiet urgency of every footstep. In that moment, you remember that a single delayed decision can change an outcome.
Having spent decades as a clinician and neurosurgeon, and more than 16 years as superintendent of China Medical University Hospital (CMUH), I believe leadership is reflected in a team’s ability act quickly, safely and consistently under pressure.
When we talk about smart health care, I ask one question: Does it make care more humane and more reliable? Technology must reduce friction, reconnect workflows and protect the people who protect patients—physicians, nurses, pharmacists and every member of the multidisciplinary team.
A Philosophy Formed in the Operating Room and Tested in Management
My clinical life trained me to make decisions with incomplete information, and to respect how quickly small delays can become irreversible harm. I have seen highly trained teams lose precious minutes simply because vital signals lived in different systems and no one had a shared, reliable picture of what mattered most. Those moments shaped my approach to leadership: Don’t ask people to work harder to overcome complexity—reduce the complexity itself, clarify ownership and build workflows that make reliability the default, not heroics.
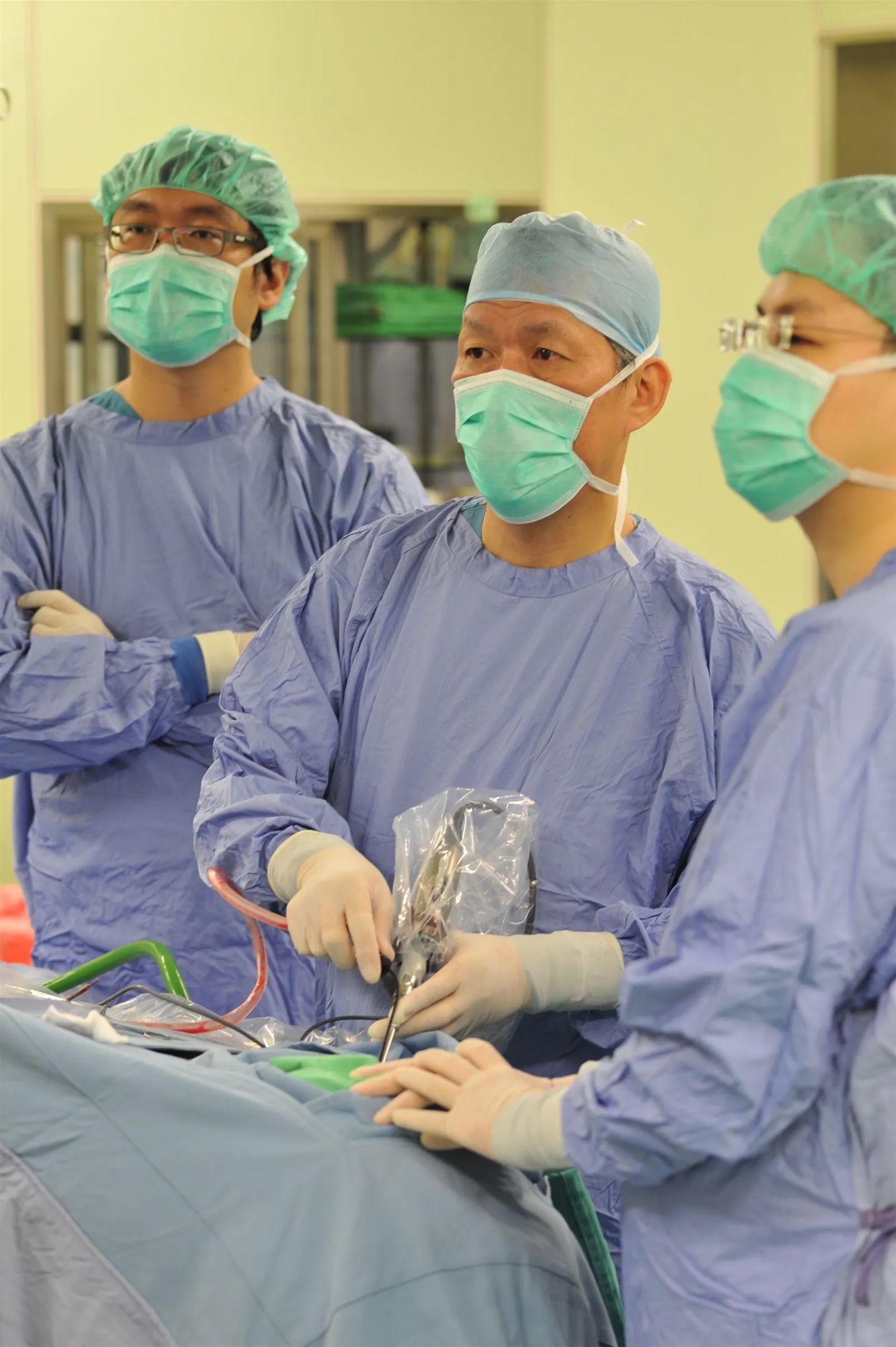
Superintendent Der-Yang Cho in the operating room.
So, we built a culture of continuous improvement—what we call “learning through action.” We treat external frameworks as stress tests, not finish lines, because they expose whether our rules, like stable data definitions, clear clinical ownership and escalation, actually hold and can be improved.
When those external lenses translate into everyday operating rules—standardized definitions, traceable workflows, measurable outcomes and accountability—innovation becomes repeatable. That is how we scale new ICU capabilities safely as a system, instead of relying on heroic individual effort.
From Data Silos to a Living System: Why We Chose Critical Care As Our Breakthrough
Every hospital struggles with data islands—information scattered across devices, systems and departments. When data is fragmented, teams work harder to see less, and critical signals can be missed.
That is why we chose the ICU as the starting point for digital transformation. Nearly 70 percent of our life-supporting devices are concentrated there, and the outcomes are measurable. With my support, clinical leaders, nurses, pharmacists, IT members and engineering staff met weekly over six months to map workflows, align data definitions and decide both what would trigger action and who would own that action. We agreed we would not scale beyond the pilot until three indicators moved in the right direction: time-to-alert, time-to-escalation and documented compliance with our escalation protocol.
We began with workflows that every clinician recognizes: sepsis screening, stroke alerts, ventilator management and high-risk deterioration. The principle was simple: fewer screens, faster alignment and clearer accountability.

China Medical University Hospital (CMUH), Taichung, Taiwan.
HiThings Tele-ICU: Building an ICU "Command Center" that Works for Clinicians
The core of our critical-care transformation is the HiThings Tele-ICU "command center." It did not start as a technology project. It started as a commitment to reduce cognitive load and help ICU teams act with clarity when seconds matter.
From the beginning, we designed HiThings Tele-ICU as an end-to-end operating model: an Internet of Things (IoT) foundation that unifies real-time feeds from more than 1,200 devices and core hospital systems (EMR, labs, imaging) through standards such as Fast Healthcare Interoperability Resources (FHIR), which then turns that stream into actionable context. FHIR is a health care data standard that helps different systems share structured clinical information consistently.
Reliability is non-negotiable in critical care. We engineered the platform for high availability and near-real-time messaging, so clinicians can trust it during peak ICU demand.
To get there, we brought multidisciplinary teams together and redesigned the workflow before writing code. We built two clinician-facing views:
- An ICU Overview Panel that provides unit-wide, real-time situational awareness (beds, risk levels, infection indicators, equipment status).
- A Patient Digital Twin Panel that consolidates real-time signals—vitals, labs, imaging and AI risk predictions—into an intuitive patient-shaped 3D view. The goal is not visualization for its own sake. It is faster clinical sense-making from a single, coherent patient picture. Think of it as an integrated clinical canvas—one place where signals, context and risk are organized for faster decisions.
Together, they give teams both the "forest" view of the unit and the "tree" view of each patient—without forcing clinicians to chase information across multiple screens.

HiThings Tele-ICU unifies IoT, AI-CDSS, digital twin visualization and teleconsultation. In the center is Superintendent Der-Yang Cho
We ensured the system to match how clinicians actually work today: web-based, secure and accessible across devices, with role-based access, audit trails and teleconsultation "anytime, anywhere. " This ensures expertise can reach the bedside without delay.
Inside the command center, six clinically validated decision-support services (AI-CDSS) are woven into daily ICU work—not as separate apps, but as prompts that help teams align faster. Some are built for minutes: Sepsis AI, STEMI AI and Stroke AI each flag high-risk patterns early and activate standardized pathways. Others support the long fight: ARDS AI tracks severity around the clock, Nutrition AI personalizes targets for critically ill patients and Generative AI drafts structures summaries and notes for clinician review. Every alert is paired with a defined clinical owner—so AI signals translate into accountable action, not noise.
By embedding these tools inside the workflow rather than as standalone apps, we keep clinicians in one place. Signals, actions and accountability stay aligned.
What Changes When the System Becomes Proactive
The most meaningful transformation is psychological. Clinicians move from reacting to patient deterioration to anticipating it.
Instead of waiting for a crisis, teams can see who is trending toward risk and intervene earlier, with shared visibility across disciplines.
We are not replacing clinical judgment. We are restoring it by returning time, attention and a coherent picture of the unit, so clinicians can act with clarity and confidence.
Instead of chasing numbers across systems, teams can focus on decisions, communication and compassionate care.
Measurable Outcomes: Saving Lives, Reducing Burnout, Improving Quality
In health care, credibility comes from outcomes and from being transparent about how we measure them.
As HiThings Tele-ICU rolled out in phases across multiple adult ICUs over the course of a year, we tracked outcomes and workload indicators through internal pre/post monitoring. The goal was practical: Do teams see risks earlier, act faster and document less—without adding clicks?
Across participating units, overall ICU mortality fell by 6.3 percent relative to the pre-implementation baseline in the same ICUs. At our current volumes, that corresponds to an estimated several dozen additional lives each year—an operational signal we continue to monitor as we scale. As adoption expands, we validate performance across units and case mixes, refining pathways when the data tells us to.
For time-critical conditions such as stroke and ARDS, we tracked time-to-alert and time-to-escalation as operational indicators, aiming to surface high-risk signals earlier and align teams faster.
These gains come from a closed loop: IoT data feeds the AI services, the digital twin makes risk visible and teleconsultation scales expertise when staffing is tight.
Most importantly, teams report less alarm fatigue and more confidence that critical signals will be seen, understood and acted on. As one ICU nurse told me, "I’m spending less time hunting for information and device inventory, and more time caring for patients."
 HiThings Tele-ICU enables real-time teleconsultation and a shared ICU view—so teams can align quickly and escalate with clarity.
HiThings Tele-ICU enables real-time teleconsultation and a shared ICU view—so teams can align quickly and escalate with clarity.
Building the Talent Engine: Investing in People Who Can Scale Innovation
Hospitals cannot "buy" transformation. They have to build it—with people, process and governance.
Under our strategy, CMUH invested in capabilities to scale: an AI center, big-data infrastructure and more than 80 engineers working side-by-side with clinical owners. We review real ICU cases together—what fired, what was missed, who owned the escalation and what we will change by next week.
Interoperability is not optional. We align vendors and systems to shared standards, so data becomes real-time, reliable and usable for care.
With this foundation, we can extend critical-care expertise across the China Medical University Healthcare System—from our Taichung medical center to regional hospitals—through teleconsultation and shared dashboards, without diluting standards or overloading frontline staff. In practice, this means a hub-and-spoke model across our network: bedside teams can request rapid input, share the same real-time view and document decisions consistently.
Recognition is Meaningful When It Reflects Real Capability
HiThings Tele-ICU earns external recognition only when it delivers measurable results and durable operations. Benchmarks such as the Newsweek AI Impact Awards APAC and Newsweek World’s Best Smart Hospitals—together with HIMSS digital maturity assessments—serve as checkpoints, testing whether our governance, interoperability and frontline adoption hold up under scrutiny. We don’t chase trophies; We chase safer care, a healthier workforce and systems that remain reliable long after the headlines.
The Future: A Hospital That Learns, Adapts and Stays Human
When people ask what I want CMUH to become, I give a simple answer: a hospital that learns at the speed of change while staying grounded in human care.
HiThings Tele-ICU is not the end. It is a foundation—an architecture for real-time care, interdisciplinary collaboration and continuous improvement.
In the ICU at 3 a.m., nobody cares about slogans. They care about whether the system works.
Our job is to make sure it does.
Related news from Newsweek: Redesigning Critical Care for the Modern ICU - Newsweek



