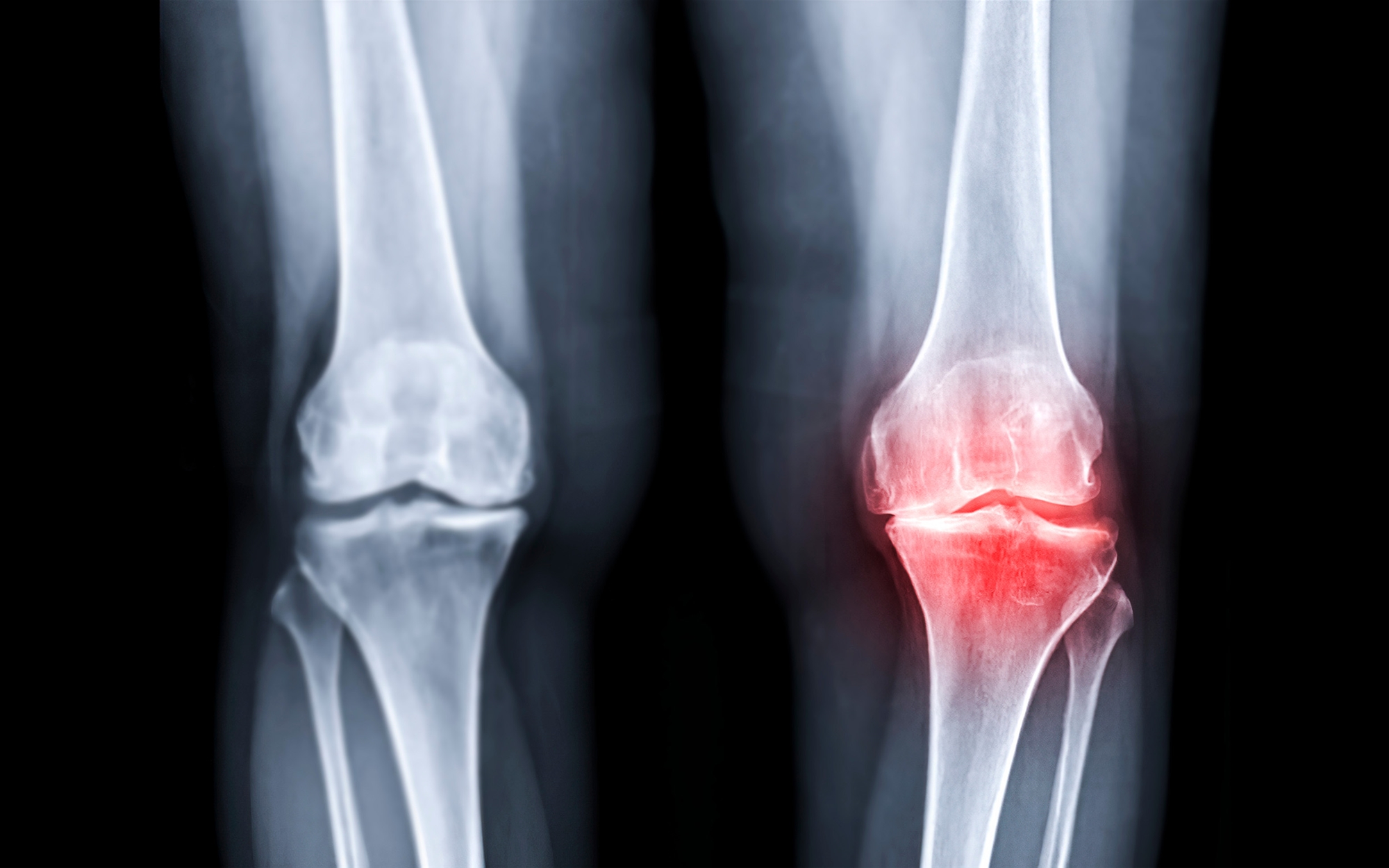
The structure of knee joint
Knee joint contains bone, ligament, joint cavity, meniscus, patella, cartilage, femur, and tibia. Because of its complex structure and weight-bearing capacity, knees are the most commonly injured joints. Osteoarthritis is a joint disease that mostly affects cartilage. Cartilage is the slippery tissue that covers the ends of bones in a joint. Healthy cartilage allows bones to glide over one another. It also absorbs energy from the shock of physical movement. The breakdown of cartilage causes bones within cartilage to rub together ( bone-on-bone ).
What is Osteoarthritis?
Osteoarthritis occurs when the cartilage that cushions the ends of bones in your joints deteriorates over time. The smooth surface of the cartilage becomes rough, causing irritation. Eventually, if the cartilage wears down completely, you may be left with bone rubbing on bone — causing the ends of your bones damaged and joints painful.
Joint pain and stiffness are the main symptoms of arthritis. Pain, swelling, and loss of motion result. The joint may lose its normal shape over time and become deformed. Osteoarthritis is a joint disease that mostly affects cartilage, a slippery tissue covering the end of the bones in a joint. Its symptoms often develop slowly and deteriorate over time. Signs and symptoms include: painfulness, tenderness, stiffed joint, loss of flexibility, grating sensation, and bone spurs looking like a swelling hard lump.
Factors increasing your risk of osteoarthritis include
- Age : Osteoarthritis typically occurs within older adults especially to people over 40.
- Sex : Women are more likely to develop osteoarthritis, though it isn't clear why.
- Obesity : Carrying more body weight places more stress on your weight-bearing joints, such as your knees, so obesity has been linked to be an increased risk factor of osteoarthritis.
Treatment
- Medications treatment include: Acetaminophen, Nonsteroidal –anti-inflammatory drugs ( NSAIDs ), and Visco- supplementation. Injections of hyaluronic acid derivatives (Hyalgan, Synvisc) are also used for pain relief and symptom control.
- Physiotherapy
- Arthroscope examination and treatment
- Total knee arthroplasty
What is Knee Replacement Surgery?
Knee replacement surgery — also known as total knee arthroplasty (ARTH-ro-plas-tee) — helps relieve pain and restore functions of severely ill knee joints. During knee replacement, a surgeon cuts away damaged bone and cartilage from your thighbone, shinbone, and kneecap; and replaces it with an artificial joint ( prosthesis ) made of metal alloys, high-grade plastics, and polymers.
The first artificial knees are no more than crude hinges. With the advancement of technology, you and your doctors have a variety of designs to choose from base on your age, weight, activity level, and overall health condition. Most knee replacement joints are capable of replicating the natural ability of your knees to roll or glide as it bends.
In joint replacement surgery ( arthroplasty ), your surgeon removes your damaged joint surfaces and replaces them with plastic and metal devices called prostheses. The hip and knee joints are the most commonly replaced joints. But today implants can replace your shoulder, elbow, finger or ankle joints. How long your new joint lasts depends on how you use it. Some knee and hip joints last as long as 20 years. Joint replacement surgery resumes your activity and provides a pain-free lifestyle. With smaller hand joints, it helps improve appearance and comfort and mobility of your joints. Joint replacement surgery carries a small risk of infection and bleeding. Artificial joints can wear or come loose, and may need to be replaced eventually.
The care after knee replacement surgery
-
Post-operation care - In Hospital
Your knee will be wrapped in a bulky bandage. There may be a fine plastic drainage tube running from the wound. This is to drain any residual blood from the operation. You may have a knee support on your leg to stabilize it when you are not doing your exercises. The surgical wound is painful but your attending physician would prescribe pain killers or injections to relieve such pain; you may request for more pain control if the condition gets worse. General anesthetic will slow you down, make you a bit clumsy and forgetful for about 24 hours. The nurses will help you with everything you need until you are able to do things on your own. Do not make important decisions during this time because your condition could greatly affect your decisions.
The physiotherapist will teach you important exercises and you will learn to walk using walking aids. The occupational therapist will show you how to do many daily tasks such as dressing and washing. The physiotherapist may arrange some therapy for you to work on after you are discharged from the hospital. The discomfort of the operation makes it difficult for you to urinate and empty the bladder. If you cannot urinate properly six hours after the operation, inform our medical staff immediately.
There is a simple adhesive dressing placed over the wound; a day or two after the operation, our medical staff will pull out the wound drain and remove the stitches 10-12 days later. For cleansing, wash around the dressing for the first 10 days. It will be all right to wash and rinse the wound as soon as the dressing is removed. Wash with soap and warm tap water, not salted water. Shower or bath is permissive once the wound is healed. Return to the hospital for the appointment with your orthopedic physician 6 weeks after the operation.
- After - At Home
When you go home, you will be able to move around the house and stairs. It is very important that you continue the exercises instructed to you. You will not be able to go shopping for the first few weeks after you go home. Please make arrangements for friends or family to shop for you. Your knees will continue to improve for at least six months. Some people say that it takes this much of time for your new knee to become part of you. You must not drive for two months after you leave hospital. You will not be able to perform an emergency stop as quickly as you used to do. How soon you can return to work depends on your job. For example, you can return in 6 weeks after the operation if driving is not a must; however, you should not proceed to manual work after a total knee replacement.
Possible Complications
As with any operation under general anesthetic, there is a very small risk of complications related to your heart or lungs. The tests that you have before the operation is to ensure your undergoing the operation in the safest possible way and to lower the risk of complications down to zero.
Complications occur in about 5 out of 100 operations. Wound infection sometimes happens. You will be given antibiotics to prevent this. Blood clots may develop in the veins of your calf ( deep vein thrombosis -DVT ). To prevent you from having such a complication, combined treatments like injections for thinning blood, compression stockings, and foot pumps are used and prescribed.
More serious complications like damages of knee joint, nerves, and blood vessels rarely occur during the operation; if it does happen, you will be required to undergo another operation.
Artificial joints last for years; however, they can become loose and painful after years of use. A further operation may then be necessary.
General Advice
Since this is a mediocre operation, when there is Osteoarthritis, we generally suggest patients to undergo a knee joint operation. Here we have provided a general guide for you to better understand the disorder but do remember this: all hospitals and surgeons vary with their own policies. Get in touch with our medical staff if there is any inquiry concerning you.